Breakthrough Trips
Psychedelics are a mental health game changer
By Kai Grady, Jack Mittemeyer, Maryssa Rillo, Juliette Smith & Patrick Waechter
Warning: This story contains descriptions of suicidal ideation and the use of psychedelic drugs and may be disturbing to some.
Twenty-seven-year-old Mitchell Maldonado was diagnosed with chronic depression over a decade ago. Since then, doctors have prescribed him over 25 psychiatric medications—he’s currently on three. And he’s seen more therapists than he can count.
The drugs failed to heal Mitchell’s brain. He became so entrenched in his own despair, only the thought of killing himself offered him relief.
“I got to a point where suicidal ideation and the thought of suicide was very oddly calming to me,” he said. “I knew it was an option and it was an easy way out. I don’t remember a time where I didn’t think like that, even as a little kid.”
Out of options, Mitchell turned to Facebook and made a plea for help.
On July 13, 2021, he wrote: “If I do indeed perish someday due to my mental health struggles, blame the healthcare system, not me.”
A friend saw Mitchell’s post and alerted him about Phoenix Nest Community Project, a Chico clinic that heals mental illnesses with the only psychedelic therapy that is legal in California—ketamine. Mitchell called Phoenix Nest, and was sitting cross-legged and barefoot the very next day at his first ketamine therapy session.

“A lot of patients come in here and they go, ‘Oh my God, I don’t want to see another psychiatrist or therapist. I am sick and tired of it, it doesn’t work. I feel worse after therapy,’” said Dr. Daniel Rieders, a co-founder of Phoenix Nest. Dr. Rieders is also a cardiologist and a renowned expert in integrative medicine. “When people have illnesses, this healing has to be done. Psychedelic therapy will save the health care system trillions of dollars because of the mind-body connection.”
The use of psychedelics began way before kids started using them to get high at parties, before scientists started studying their effects on the brain and way before the government declared a “War on Drugs.”
Indigenous people of the Americas have used psychedelics derived from plants for thousands of years. By 1912, scientists started synthesizing hallucinogenic drugs for medicinal reasons including, MDMA (1912), DMT (1931), and acid (1938). In the 1950s, psychiatrist Humphrey Osmond and author-philosopher Aldous Huxley coined the term “psychedelic,” which is defined as mind manifesting or mind expansion.
By the 1960s, with Dr. Timothy Leary and Dr. Richard Alpert’s Harvard Psilocybin Project, psychedelics started gaining popularity for recreational use. Leary touted the benefits of psilocybin and LSD for the brain and urged the public, “turn on, tune in, drop out.” The U.S. government saw this as a threat to the social order and by 1971 declared "war." Psychedelics including MDMA (“ecstasy”), psilocybin (“shrooms”), LSD (“acid”) and peyote were banned and listed as Schedule I drugs with no medical use.
Psychedelics have historically been associated with recreational use, but that view is shifting.
Ketamine was originally developed in 1962 as an anesthetic for animals and has been used for decades in hospitals for sedation and pain management. Now, mental health clinics around the U.S. are recognizing the drug’s unique psychotropic benefits that allow patients to experience deep healing of past traumas.
Psychedelic medicine is no longer only the domain of shamans and recreational drug users; they are now in the hands of trained psychotherapists and doctors. People tethered to pharmaceutical antidepressants their entire lives are finally experiencing true relief from the very “drugs” we were all told to stay away from.
“The side effect of this treatment is people find joy in their life, and they’re spreading that joy to their families and community and tribes,” Rieders said.
As more people turn to these alternative forms of medicine, states like Iowa, Maine, and California are considering legislation that would decriminalize psychedelics. In California, advocates and politicians are fighting about what it means to actually decriminalize these substances.
Activists for total decriminalization argue that corporate influence is more focused on the potential market for psychedelics than the humans who need healing. The battle between activists and corporate interests is ongoing.
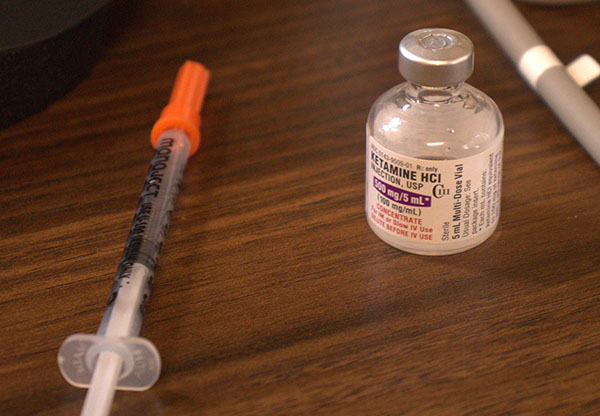
A vial of ketamine and a syringe.
FDA scientists are also studying and testing the benefits of MDMA on the human brain. Many people still associate psychedelics with hippies, tie-dye and people thinking that they can fly. They aren’t educated on the medicinal properties of these drugs. With this lack of education comes societal stigma, which means many people who struggle with their mental health are ultimately denied potential life-healing experiences.
Mitchell’s story is testimony to the benefits of psychedelic therapy. As he prepared for what would be his third ketamine treatment, he invited us to Chico to see his healing firsthand at Phoenix Nest.
Psychedelics vs. Pharmaceuticals
The most common treatment for those struggling with mental health are pharmaceuticals. Pills, pills, pills. Patients enter a cycle of suppressing their symptoms when what they desperately need is healing. Dr. Nicholas Brüss is a licensed psychotherapist in Los Angeles, specializing in integrative, ketamine-assisted psychotherapy, and internal family systems. Certified in Mindfulness Facilitation at UCLA’s Mindful Awareness Research Center, Brüss is also a therapist at the Los Angeles site for the MAPS-sponsored Phase III clinical trial of MDMA-assisted psychotherapy for PTSD.
Brüss said pharmaceutical drugs only mask people’s issues.
“Psychiatrists are in a position where they are treating symptoms,” he said. “Probably most people today don’t even have the expectation that they are going to take a pharmaceutical drug and then be healed.”
Mitchell fell into what felt like a never-ending cycle of trying pill after pill. The process of finding the right balance of medications was essentially trial and error.
“It takes so long to get the right one. It’s just experimentation, unfortunately,” said Mitchell. “The biggest problem with a lot of them is they take a month to start working, and some people don’t have a month.”

Dr. Nicholas Brüss pauses to reflect during an interview at Café Gratitude in Venice, California.
Unlike pharmaceutical drugs, psychedelic-assisted therapy heals a patient rather than simply covering up their symptoms. Psychedelics help patients open up to their trauma and get to the root cause of their problems. People who have been weighed down by unspeakable trauma are finally able to rebuild their lives.
“We’re not giving them things to cover up or kind of get through, but rather we’re giving people these medicines to help people open up to these experiences, get to the roots of it,” Brüss said.
Psychedelic educator and activist Dr. Larry Norris, who co-founded Decriminalize Nature, a non-profit organization based in Oakland, California, said that misconceptions are a significant reason for many people’s opposition to psychedelics.
“The materials we're working with are oftentimes done in a sacred manner,” he said. “Some people have recreational experiences but for the most part people are doing this for healing, sort of a model for personal and spiritual growth.”
From the ashes: Phoenix Nest
Driving up from Sacramento, passing through the “goldfields” into Butte County, the sky filled with smoke. That was our primary indication that once in Chico, we were less than 20 miles from where the Dixie Fire was burning and growing, over 240,000 acres. By early August, it had become the second-largest wildfire in California history.

"Homo Deus" by Martin Stensaas and Sunny Strasburg. This painting hangs in Dr. Rieders' office at Phoenix Nest.
We could smell the burning timber when we got out of the car, but pushing open the office door of Phoenix Nest, we entered another world. The clinic’s corridors radiate a clean, minimalist design with trippy, maximalist artworks on the walls—vibrant geometric designs, fractals, a chimpanzee in a ceremonial robe—all provided by the gallery Phaneros Art in nearby Nevada City. Two private treatment rooms provide bohemian cushions on the floor and heavy drapes to shut out the light. There is also a zen room with a Japanese rice paper screen, Buddhist statues, and a gong. The entire place smells delightful, relaxing, not at all like smoke. Everyone, including Mitchell, was barefoot.
Phoenix Nest is not your average doctor’s office.
This is a community project for the deep, holistic healing this area has needed for a long time. The 2018 Camp Fire devastated Butte County, destroying more than 150,000 acres. Maybe that’s why they seem so unfazed by Dixie.
In the aftermath of Camp, Alexandra “Alex” Kriz, began planning for a utopian, drug-free community of fire survivors. That’s when she came up with the name Phoenix Nest. The idea for a ketamine clinic began only in April, when she reached out to her friend, Dr. Daniel Rieders.

Dr. Daniel Rieders, seated on the waiting room floor, welcomes a new patient to Phoenix Nest.
Dr. Rieders recounted the story.
“We talk all the time about how the police, the fire, all the people are so traumatized here and toxified,” he said. “She called me on April 10 and said, ‘Let’s do a ketamine clinic in Chico,’ and I said, ‘Heck yes.’”
They were open by June 1.
Mitchell came to Phoenix Nest with depression, anxiety, and suicidal ideation. Others have come to them for help with PTSD or addiction. They’ve also treated couples who just wanted to rekindle their intimacy. Rieders sees his patients as more than their condition. “We don’t really treat those things,” he said. “We treat humans.”
Ketamine is often administered in more traditionally clinical settings, but Rieders sees value in offering this treatment in a ceremonial way at Phoenix Nest.

In the waiting room at Phoenix Nest: a Himalayan salt lamp; a laminated chakra awareness guide; a copy of local weekly rag, the Chico News & Review.
“Every session we do in sacred space, in ritual, and we bring in smell and sound as part of the healing space and love,” he said. “A lot of big love.” That’s true. During our visit, several times we saw patients emerge from treatment rooms. They saw Dr. Rieders or Alex, and they just went right in for a hug—a real, actual long hug.
That’s part of where the community project part comes in. “We create a family. This is the Phoenix Nest Community Project,” said Alex. “When I create a community, I like to hug my community members.”
Ketamine therapy at Phoenix Nest is $600 per session, but no one is turned away if they can’t pay. “Half of the sessions we do for free,” said Rieders. Like a true community project, the patients who pay offset costs for those in need.
Rieders discussed how this community, so often in the throes of disaster and turmoil, faces a desert of mental health resources.
“They just haven’t had access because there’s so much stigma to getting help. People are suffering in silence,” he said. “We’re just opening access because ketamine is legal, to get people in and on a healing path.”
Rieders supports decriminalizing other psychedelics for healing purposes, with supervisory stipulations. “There are all these other substances that are very powerful and healing and illegal for the most part, and it’s a problem,” he said.
Who’s talking about psychedelics?
Who isn't ?
Use this interactive soundboard to hear a chorus of different folks discussing their personal psychedelic breakthrough experiences.
Voices represent seven men, five women, and one non-binary person, ages 26 to 62, from eight U.S. states, Canada, and the United Kingdom. All audio was recorded with permission during multiple live interactive social audio conversations on Clubhouse, July 12-20, 2021.
California debates decriminalization
About an hour south of Chico, lawmakers in Sacramento debate the future of psychedelics in California.
State Sen. Scott Wiener (D-San Francisco) introduced SB 519, which would effectively decriminalize most psychedelics in the state. The bill has passed the State Senate and is making its way through the assembly.
“The senator is hoping this bill will benefit people who are suffering from mental health issues, like complex trauma, PTSD, anxiety, depression, who could potentially seek supported treatment through psychedelics,” Catie Stewart, Sen. Wiener’s director of communications, said.
“The senator is hoping this bill will benefit people who are suffering from mental health issues, like complex trauma, PTSD, anxiety, depression, who could potentially seek supported treatment through psychedelics.”
Some California representatives see things differently. A representative of Assemblyman Tom Lackey (R-Palmdale), who voted against SB 519 in committee, called the bill a “threat to public safety.”
Moreover, the latest iteration of SB 519 includes an amendment putting possession limits on certain drugs that leaves some of the bill’s original supporters feeling lukewarm about the prospects, including the co-founders of Decriminalize Nature.
Dr. Larry Norris and Carlos Plazola’s organization was heavily involved in Oakland’s fight to decriminalize psilocybin, or “magic mushrooms.” Oakland City Council passed that measure unanimously in June 2019.
Norris said that imposing possession limits contradicts their goal of abundance.
“When you start putting limits on it, unfortunately, that creates a situation where it's not really decriminalized,” he said. “Oftentimes, that hits certain communities, low-income communities, marginalized communities harder because that's where the police enforcement is going to happen.”
Plazola said that sponsors of SB 519 knew months ago that the addition of limits would later become a key component of the bill’s approval.
“This is really being driven by deep pockets with the intention, ultimately, to profiteer wrapped within a cloak of benevolence,” he said.
Though the bill seems to be a step in the right direction, advocates like Decriminalize Nature argue that people should have the right to plant medicine without limits.
“What decriminalization means to us is really what decriminalization should mean in general, which is to remove any criminality associated with that substance,” said Plazola.
Those deep pockets he’s referring to belong to funders of the New Approach PAC, among them David Bronner of Dr. Bronner’s Soap, Dan Lewis of Progressive Insurance, and Sean Parker of Facebook. New Approach has campaigned for recreational marijuana in states across America since 2014. They had their first success with psychedelics in Nov. 2020, when Oregon voters approved Measure 109 to offer legal supervised psilocybin therapy in the state by 2023.
The sharks are swimming because there’s chum in the water. According to Data Bridge Market Research, the psychedelic drug market size is expected to reach more than $10 billion by 2027.
There are internal arguments in the world of psychedelic activism, but regardless of each group’s motivation, all of them want to end the war on drugs and provide safer access to psychedelic healing.
California’s SB 519 still has a ways to go. The bill faces two more hearings in the state Assembly in the Public Health and Appropriations committees before moving to the Senate floor. Hearing dates have not been set. It is also currently unclear if Gov. Gavin Newsom (D) would sign the bill.
Psychedelic Legislation by State
Law Passed: Supervised Use
Law Passed: Medical Research
Law Passed: Reduced Penalty
Legislation In Process
Legislation Failed
Law Passed: Supervised Use
Law Passed: Medical Research
Law Passed: Reduced Penalty
Legislation In Process
Legislation Failed
To desperate veterans,
Jesse Gould throws a line

Jesse Gould, former U.S. Army Sergeant and founder of Heroic Hearts.
Former U.S. Army Sergeant Jesse Gould said SB 519 “could do more” but also called it a “step in the right direction.” His organization Heroic Hearts co-sponsored the bill. Heroic Hearts provides veterans in need of mental health services with a direct link to resources for psychedelic treatments only available outside of the United States.
Coming out of the war, Jesse thought he was fine until he started having panic attacks.
“I would lie in my room and stare at the ceiling because there was nothing I could do that would bring any sort of color or anything to my life,” he said. “I had the sudden realization that I was miserable more days than I was happy.”
"As a country we have to decide, will we classify these patriots as criminals or send them to other countries to pursue these mental health treatments they are already pursuing?"
Jesse found his healing by accident, listening to “The Joe Rogan Experience.” After hearing the podcast’s episode about the ancient Peruvian tradition of ayahuasca, he was inspired to research the ritual’s cultural history and testimonials of healing. Then, he booked a one-way ticket to Peru to try it for himself.
Ayahuasca is a brew prepared by boiling the vines of Banisteriopsis caapi and the leaves of Psychotria viridis. The leaves contain N,N-Dimethyltryptamine, or DMT. Many users report life-changing experiences. Some say they meet God.
After his first ayahuasca ceremony, Jesse found the clarity he needed to process his trauma. For the first time in a long time, he felt like his brain wasn’t “out to kill him.”
Returning from Peru, Jesse was moved to share this remedy with his fellow soldiers in need. Through Heroic Hearts, he offers veterans a supportive funnel to reach trusted practitioners and retreats in Peru or Mexico.

Jesse Gould at an ayahuasca retreat in Peru.
Credit: Pablo Genovesio
Jesse put his life on the line for the United States and acquired mental trauma along the way. Laws banning psychedelics fail veterans who are desperate for relief. Rather than receiving the help they need here in America, they are forced to travel to another country for treatment.
“As a country we have to decide, will we classify these patriots as criminals or send them to other countries to pursue these mental health treatments they are already pursuing?,” Jesse asked.
Heroic Hearts has a waitlist of over 700 veterans in need of treatment.
Mitchell’s got jokes
Mitchell was 14 when he was first diagnosed with chronic depression. Since then, he’s found it impossible to hold onto a job or keep up with a romantic relationship. He receded into complete isolation, avoiding his friends and shutting himself inside. Not because of COVID concerns but rather because of debilitating agoraphobia, he hadn’t been to the supermarket in almost a year.
His third ketamine appointment was scheduled for 11 a.m., but he was already in the waiting room when we arrived at 10:46. Alex, his integration coach for the session, led him down the hall and into the treatment room.
She took his blood pressure and went down the list—drinking and drug habits, how much sleep, all the basics. They discussed Mitchell’s previous behaviors and Alex checked in with him to see if he had any suicidal thoughts since their last session. “None.” Alex cheered. This is a huge win.
Alex moved closer, and Mitchell shifted into meditation pose—eyes closed, legs crossed, palms laid up on his knees. Alex wafted several essential oils near Mitchell’s nose, as he breathed deeply and intentionally. She rubbed a small bit of each one on his wrist. Then, she had him lay down and gave him noise-cancelling headphones, a blindfold, and a purple blanket for his feet.
She pulled the curtains closed, and Laura “Lori” Moreno, a registered nurse, came in to administer the ketamine. Mitchell didn’t flinch as the needle went in. In a state of complete relaxation, he was basically asleep for about 45 minutes. Alex and Lori stayed by his side the entire time.
Lori left and returned with a cup of hot tea. In a soft voice, Alex told Mitchell it was time to wake up. He raised to a sitting position. At first, he looked tired, even bewildered. When he saw Alex, his face lit up. He smiled, ear to ear, a pure, genuine smile. Alex welcomed Mitchell “back” and began his integration session. Like two best friends, they laughed through trauma.

Mitchell Maldonado cracking jokes after his third session of ketamine therapy.
“I was in an active state of self-hatred,” said Mitchell. They both cackled.
“Sometimes, we can feed our own enemy, though,” said Alex. “It’s OK to feel funky, but not every day.”
Mitchell joked—“Well, James Brown, he was funky arguably every day of his life.”
Mitchell’s telling jokes about the “Godfather of Soul."
They talked about what he does to care for his soul. Alex told him he should dance. Mitchell laughed and said, “No, no, nooooo.” He doesn’t dance, but he’s played the guitar since he was 7. He plays during his upswings. He’s been playing more lately. Alex advised him to play songs with good lyrics and positive intentions.
“Those vibrations matter,” she said.
Mitchell’s third session was a success.
MDMA: The next frontier?
Ketamine is the only psychedelic therapy that is currently legal throughout the United States—but with promising news about MDMA, that may soon change. MDMA, commonly known as “ecstasy,” affects the brain differently than ketamine.
“Ketamine works on the NMDA receptor,” said Dr. Daniel Rieders. “A lot of the other drugs work on the serotonin receptor. That’s a different kind of healing, a different kind of experience.” The NMDA receptor is connected to memory, but the serotonin receptor is more directly connected to pleasure.
"Many [pharmaceutical] drugs are given to sedate or to manage symptoms. MDMA and other psychedelics, in conjunction with psychotherapy, really get at the root causes."
The Multidisciplinary Association for Psychedelic Studies (MAPS), a leader in psychedelic research, is conducting clinical trials studying the effects of MDMA on patients with PTSD.
MAPS was founded by Rick Doblin, an American drug activist. He saw the therapeutic value of psychedelics and started a nonprofit that advocates for the legalization of psychedelics for therapeutic use.
Under the guidance and regulations of the U.S. Food and Drug Administration (FDA) MAPS holds MDMA clinical trials all over the United States, Canada, and Israel. These studies are possible because of participants who volunteer to undergo the therapy. The volunteers must be 18 years or older and experiencing symptoms of PTSD for at least six months.
The therapists create a healing safe place where people can re-experience past traumas and walk away with a different meaning, to process things in a new way without having the same rigid thought processes we all habitually fall into.
Brüss explained that MDMA, when taken in a controlled situation, allows patients to self-advocate for inner healing intelligence. The therapist works with the participant to understand what their trauma is and the events that led to it. The psychedelic helps decrease fear and increase trust.
“Many [pharmaceutical] drugs are given to sedate or to manage symptoms. MDMA and other psychedelics, in conjunction with psychotherapy, really get at the root causes,” Dr. Nicholas Brüss said.

Dr. Nicholas Brüss works with MAPS on MDMA clinical trials and offers ketamine therapy to individual clients.
These clinical trials have shown promising results. After four months of MDMA-assisted therapy, 67% of participants no longer show PTSD symptoms.
Evidence, both in testimony and in measurable statistics, suggests that psychedelics heal the human mind. MAPS clinical trials are currently in Phase III, the final stage before a drug can be approved by the FDA for controlled use. That means MDMA is on track for FDA approval by 2023.
Mitchell is excited to live his life.
If you met Mitchell Maldonado today, you would never guess he struggled with debilitating anxiety and depression his entire life. He started getting out of the house and seeing his friends. He’s been working on a project, restoring a 1973 Datsun 240z. He finally made it to the supermarket.
“It was like, all of a sudden somebody turned the lights on. I’ve been in the dark for my whole life and someone turned the lights on,” he said. “I’ve felt good, not just OK, but like good, all the way until my next session.”
Ketamine saved Mitchell’s life. He no longer fantasizes about killing himself. For so long, it was all he could do just to survive. Now, he’s joyous. Dr. Rieders says they see stories like Mitchell’s all the time.
“They’re able to do this because they’ve released all the mind chatter, so all of a sudden their wise self, their higher self is there, and they have access to these other things,” he said.
Many others suffering from debilitating mental health issues are in desperate need of relief. Yet their access to an assortment of potentially life-saving psychedelic treatments is caught up in legislative debates, FDA red tape, and societal stigma. People are dying. We need to act now.
Remember that 1987 television commercial at the height of the anti-drug campaigns? A man held up an egg and said, “This is your brain.” He cracked the egg open over a hot frying pan, and it started bubbling turbulently. “This is your brain on drugs.”
Dr. Brüss offered a different perspective, one that challenges us all to think a bit more about the changing views on non-traditional treatments. “We know now what’s going on in the brain and it does not look like an egg being fried,” he said. “Choose to be open to science over stigma as a way of finding out the healing useful capacities of psychedelics for many different diagnosis.”

Mitchell Maldonado sits in the zen room at Phoenix Nest Community Project in Chico, California.
In memory of Joshi
Joshi was more than my first cousin. She was the sister I never had. I used to blacken my eyes like a raccoon and straighten my curly locks of hair as a young teen just to look like her. Joshi would stay on the phone, watching over me from across the world for hours while my mom was at work. I can still see her and her brother Ethan lying in the snow at the foot of our car as kids in protest as my mom and I packed the car to leave Glasgow and head home to Los Angeles— I had never felt as loved as I did at this moment.

Joshi and Juliette Smith, Glasgow, Scotland 2002.
At 24, she passed away after a lifelong struggle against chronic depression, high anxiety and OCD. A Fentanyl-laced drug, possibly a street-concocted Xanax or another opioid, was the answer to her years of pain.
The very fact that an opioid epidemic in the U.S. rages among people trying to self-medicate is a testament to the lack of mental health resources in the U.S.
I wish I could call her up and tell her about our findings. I wish I could tell her about Mitchell. How he smiled after his Ketamine treatment— How he found inner peace. I wish I could tell her about how Jesse was so inspired by his trip to Peru that he started his own non-profit to help other veterans suffering with PTSD. I wish I could introduce her to Dr. Rieders and Dr. Brüss and take her for treatment under their care. I wish I could offer her the same glimpse of hope that Mitch and Jesse shared.
Joshi's family went as far as to move across the world from Scotland to Florida in search of better treatment for her.
An extra sting is knowing detectives researching her case found internet searches for LSD and ayahuasca on her laptop. This led detectives of the Seminole Police Department in Hollywood, Florida to dismiss her as another drug user. To them and other detectives, she was just another number to add to the fatal opioid crisis. And I wonder how many hundreds of thousands of times more it is missed, misconstrued and misunderstood by police departments across the country.
Mark says she was interested in using psychedelics to deal with her trauma, which she knew was at the root of her mental illness. Joshi’s desperation went so far as to microdose LSD herself which her dad says wasn't effective.

Mark and Joshi Smith.
Mark and Joshi researched ayahuasca together. He says a clinic in Florida wanted $10,000 for a five-day session, an outrageous cost. They later discussed flying to Peru for an ayahuasca retreat, as long as Mark could supervise.
Mark’s biggest concern about the decriminalization of psychedelics is money and equality of access; he worries decriminalizing will only help the handful of people who can afford it. It is true that to survive and find treatment for mental illness in the current U.S. climate, you must have money. We see it time and time again, including Mitchell’s experience. Money is the sole reason why the opioid epidemic spread across the United States. Money failed his daughter, my cousin.
Just four months ago, the Florida House rejected FL 548, which would have created a legal pathway for psilocybin to be offered as mental health treatment. This could have helped people like Joshi.
“The U.S., for all its wealth, technological innovation and medical advances, is in fact among the cruellest, most ineffective places in the world to be mentally ill,” Mark wrote for the Herald, the Glasgow-based Scottish national newspaper.
Mark says psychiatrists never suggested psychedelics for Joshi. They only wanted to dole out drug company antidepressants and other antipsychotics, and to increase dosages.
Joshi would have been a great candidate for psychedelic therapy. She struggled with her mental health and addiction— two afflictions that can be treated with psychedelic therapy. Unfortunately, Joshi never had a chance to meet medical professionals like Dr. Brüss and Dr. Rieders nor did she hear from the patients who found the help they so desperately needed. Joshi needed a doctor who could think beyond the dogma of the multibillion-dollar pharmaceutical industry, whose products were foisted upon her, but did nothing to help her, or the millions of others like her.
We did an enormous amount of research on the benefits of psychedelics for mental health. We’ve seen and heard from so many people who have found help from psychedelics. I am happy for them, but I can't even begin to tell you how much it makes me want to violently scream. Joshi should have had this opportunity, too.
To sign the petition or to donate, visit The Joshi Project.
